Select your region
-
Europe
-
Americas
-
Africa and Middle East
-
Asia Pacific
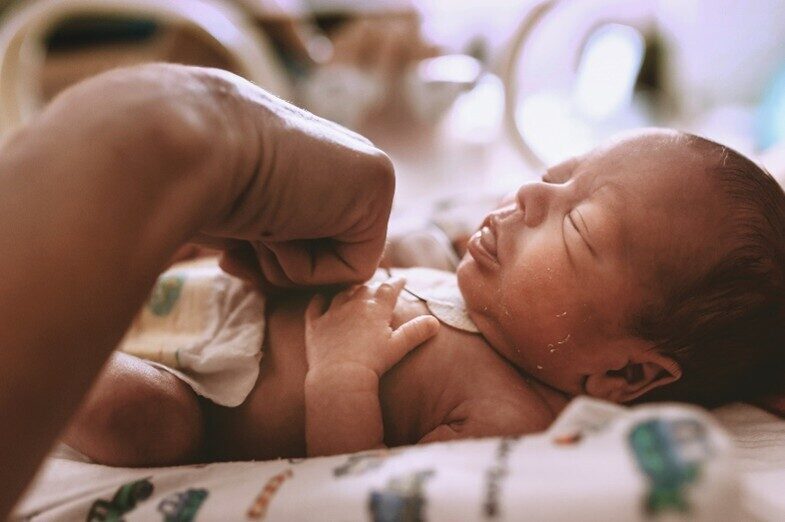
The thin, immature skin of preterm babies forms an inadequate barrier to potential irritants in the outside world and is easily damaged. For those babies spending early life in the neonatal intensive care unit (NICU), skin damage is a potentially painful by-product of life-saving monitoring and treatment. A frequent part of these babies days are nappy changes, during which their underdeveloped skin is exposed to the environment and must be cleansed. It therefore becomes imperative not to compound the distress already experienced by these infants by preserving skin integrity during nappy area cleansing.
Clinical trial data support that baby wipes can be a well-tolerated alternative to cotton wool/cloth and water for cleansing the nappy area of preterm infants, but have not been gathered extensively in preterm infants born earlier than 30 weeks’ gestation. Emerging data and our own experiences add to this evidence base to suggest that the wipes best tolerated by preterm infants are likely to be those with the fewest ingredients and therefore the fewest potential irritants.
We therefore make the following key recommendations:
- Nappy changing in preterm babies should be approached with the utmost care to minimise baby and parental/caregiver distress and preserve the integrity of the friable skin of these infants
- Decisions on skin care best practice should be made according to clinical evidence in preterm infants specifically, and in accordance with guidelines only when they are evidence-based
- Use of wipes with minimal ingredients (e.g. only purified water and grapefruit extract) for nappy area cleansing of preterm babies

Introduction
In order to understand how to support healthcare professionals (HCPs), parents and other caregivers to upskill in and deliver best practice on baby skin care, WaterWipes convened a global advisory board of 17 experts from eight countries in September 2020. The advisers highlighted that guidelines on skin cleansing from leading bodies such as the World Health Organization, UK’s National Institute of Health and Care Excellence and the American Academy of Pediatrics do not provide recommendations specific to preterm infants (gestational age <37 weeks), nor have they been updated to reflect emerging data.1–3
Our subgroup of four advisers with expertise in the care of preterm infants was therefore galvanised to develop evidence-based recommendations on cleansing preterm skin during nappy changes that are informed by the latest data gathered in premature infants and reflect their unique vulnerability.
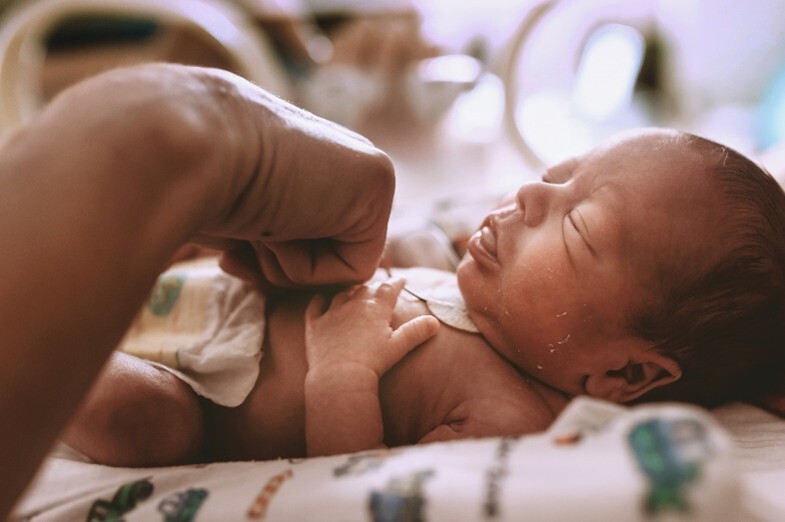
The unique features of preterm skin
The skin’s complex development begins soon after conception and continues over the first year of life.4,5 Crucial developmental stages occur towards the end of gestation meaning that, the more preterm an infant, the more vulnerable the skin is when it is first exposed to the world at birth.4,6 The drastic differences in skin quality in term and preterm infants are largely driven by the fact that the stratum corneum, the skin’s protective barrier, is thin and immature and does not form a functional barrier until 32–34 weeks’ gestation.6,7 This inadequacy of the skin barrier is demonstrated by the fact that transepidermal water loss is 15 times higher in infants born at 25 weeks gestation than in full-term infants, reducing skin hydration.8 Preterm newborns will also readily absorb topical agents applied to the skin, the effects of which are further intensified by the high ratio between body surface area to body weight.9
Below the epidermal layer, preterm infant skin also exhibits deficiency of dermal structural proteins, including collagen, making it more susceptible to oedema and blistering from friction.10,11 In addition, the protein and lipid-rich vernix caseosa is produced by foetal sebaceous glands at approximately 28 weeks—babies born at less than this gestational age do not benefit from its beneficial effects on skin pH, hydration and erythema.6
These considerations highlight the need for the development of recommendations on nappy area cleansing, which are tailored specifically for preterm babies and based on evidence gleaned in these infants rather than those born at full term.
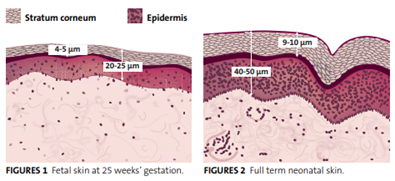
Adapted from Jackson A. Infant 2008;4(5):168-71.4
The stress experienced by preterm babies and their carers, and skin damage as a compounding factor
The challenges of maintaining the integrity of a preterm baby’s skin are not only influenced by the inherent qualities of this delicate and underdeveloped organ. For many of these neonates, the NICU is their first home. While these medical units no doubt save the lives of those babies admitted into their care, NICU babies require an average of 7.5 to 17.3 invasive procedures per day, many of which require puncture or handling of the skin that has the potential to cause damage.12 Although the relationship between skin damage and pain in premature infants has not been quantified, we know that it is painful through our experiences working with these babies.
However, it is not only these invasive procedures that have the potential to stress a preterm infant. Studies show that, for these tiniest of patients, even routine care such as nappy changing in the absence of skin damage can provoke a physiological stress response and/or behavioural disruption.13–15 Given that nappy changing can occur as often as twelve times a day in early babyhood, this has the potential to be a huge burden.16 If nappy area skin integrity is compromised, nappy changing has the potential to be even more traumatic for a preterm baby.
Compromised nappy area skin integrity can manifest as nappy rash. Nappy rash is an acute, episodic inflammatory reaction that is characterised by erythema, papules and pustules in the nappy area.17 While the incidence of nappy rash in babies born at term is generally accepted to be approximately 25%,2,18,19 data in preterm babies are limited and inconclusive.15,19,20
However, it can be hypothesised that the ineffective epidermal barrier of preterm infants may leave these infants particularly vulnerable to nappy rash compared with term babies, and that extra care needs to be taken when cleansing the nappy area of these babies.18 Our own experiences and the literature certainly suggest that, despite good understanding of how to manage nappy rash, it is prevalent in the NICU.15,18
When preterm babies are stressed, their parents and carers also suffer. The effects of this distress are not only short term, but can adversely affect the relationships between the babies and their carers, as well as the baby’s development.21,22 Therefore, we have reviewed data on the maintenance of nappy area skin integrity and prevention of nappy rash in preterm infants to recommend cleansing methods that we feel are the least likely to cause skin damage and add to the stress already experienced by these babies and their families.
Clinical data on nappy area cleansing of preterm babies
It has been known since 2012 that modern baby wipes can be as gentle on the skin of term babies as cotton wool and water.23 Moreover, cotton wool and water can be an impractical cleansing method for modern caregivers owing to considerations such as the need to access clean water, the fact that cotton fibres stick to the skin and the small size of cotton balls/pads.24
Examination of data gathered in preterm babies, as well as our own experiences, support that baby wipes can be a well-tolerated alternative to cotton wool/cloth and water.10,15,20 In fact, in a study of 130 NICU babies, perineal erythema and transepidermal water loss (TEWL) were significantly lower for infants cleansed with wipes versus cloth and water, beginning at Day 5 for erythema and Day 7 for TEWL.15 A limitation of this study is that infants with a gestational age of 23–29 weeks could not be enrolled due to their medical conditions and a reluctance of parents to provide consent to participate.15
Real-world experiences and emerging data suggest that baby wipes with the fewest ingredients may be the best tolerated as they are less likely to contain potential irritants.10,20 A US-based NICU implemented a standardised ‘perineal care guideline’ aimed at the prevention and treatment of nappy rash that included the use of baby wipes containing only purified water and grapefruit seed extract (WaterWipes® ).20 The median gestational age of the babies was 34 weeks (range: 24–41 weeks) pre-implementation of the guideline and 36 weeks (range: 23–42 weeks) post-implementation. Adoption of this guideline and these wipes containing minimal ingredients led to a 16.7% reduction in the incidence of nappy rash, a 34.9% reduction in the incidence of severe nappy rash cases and shortened duration of nappy rash by 57% (3.5 days per 100 patient-days).20 As a balancing measure, this study examined whether the use of these minimal-ingredient wipes led to an increase in fungal infections and found no such increase.20 We also believe use of small individualised packs of wipes for each neonate can further reduce the risk of infections.
Recommendations and conclusions
We would like to raise awareness of the potential distress caused to preterm infants during nappy changes and emphasise, therefore, that it is imperative to cleanse the skin using a method that does not compound this further by disrupting skin integrity. Best practice when cleansing preterm infants should be guided by clinical evidence obtained in this vulnerable population and only guidelines that are evidence-based should be considered during decision-making. We encourage HCPs, parents and other caregivers to consider using baby wipes with minimal ingredients (e.g. ultra pure water and grapefruit extract), on preterm infants for nappy area cleansing.10 We have successfully used such wipes in preterm infants as young as 23 weeks without experiencing adverse effects.20
Financial support
Financial support for the global meeting was provided by WaterWipes UC. A report was generated, which formed the basis of this document. All views expressed in this article are from the authors.
References
- World Health Organization (WHO). Pregnancy, childbirth, postpartum and newborn care—A guide for essential practice (3rd edition), (2015).
- National Institute for Health and Care Excellence. Nappy rash, (2020).
- National Institute for Health and Care Excellence. Postnatal care up to 8 weeks after birth [CG37], (2006).
- Jackson, A. Time to review newborn skincare. Infant 4, 168-171 (2008).
- Nikolovski, J., Stamatas, G. N., Kollias, N. & Wiegand, B. C. Barrier function and water-holding and transport properties of infant stratum corneum are different from adult and continue to develop through the first year of life. J Invest Dermatol 128, 1728-1736, doi:10.1038/sj.jid.5701239 (2008).
- Kusari, A., Han, A. M., Virgen, C. A., Evidence-based skin care in preterm infants. Pediatr Dermatol 36, 16-23, doi:10.1111/pde.13725 (2019).
- Kalia, Y. N., Nonato, L. B., Lund, C. H. & Guy, R. H. Development of Skin Barrier Function in Premature Infants. 111, 320-326, doi:https://doi.org/10.1046/j.1523-1747.1998.00289.x (1998).
- Hammarlund, K. & Sedin, G. Transepidermal water loss in newborn infants. III. Relation to gestational age. Acta Paediatr Scand 68, 795-801, doi:10.1111/j.1651-2227.1979.tb08214.x (1979).
- Oranges, T., Dini, V. & Romanelli, M. Skin Physiology of the Neonate and Infant: Clinical Implications. Adv Wound Care (New Rochelle) 4, 587-595, doi:10.1089/wound.2015.0642 (2015).
- Johnson, D. E. Extremely Preterm Infant Skin Care: A Transformation of Practice Aimed to Prevent Harm. Adv Neonatal Care 16 Suppl 5S, S26-s32, doi:10.1097/anc.0000000000000335 (2016).
- Visscher, M. O., Taylor, T. & Narendran, V. Neonatal intensive care practices and the influence on skin condition. J Eur Acad Dermatol Venereol 27, 486-493, doi:10.1111/j.1468-3083.2012.04470.x (2013).
- Cruz, M. D., Fernandes, A. M. & Oliveira, C. R. Epidemiology of painful procedures performed in neonates: A systematic review of observational studies. Eur J Pain 20, 489-498, doi:10.1002/ejp.757 (2016).
- Yung-Weng, W. & Ying-Ju, C. A preliminary study of bottom care effects on premature infants' heart rate and oxygen saturation. J Nurs Res 12, 161-168, doi:10.1097/01.jnr.0000387499.24428.16 (2004).
- Comaru, T. & Miura, E. Postural support improves distress and pain during diaper change in preterm infants. J Perinatol 29, 504-507, doi:10.1038/jp.2009.13 (2009).
- Visscher, M., Odio, M., Taylor, T., Skin care in the NICU patient: effects of wipes versus cloth and water on stratum corneum integrity. Neonatology 96, 226-234, doi:10.1159/000215593 (2009).
- National Health Service. How to change your baby's nappy, (2018).
- Carr, A. N., DeWitt, T., Cork, M. J., Diaper dermatitis prevalence and severity: Global perspective on the impact of caregiver behavior. Pediatr Dermatol 37, 130-136, doi:10.1111/pde.14047 (2020).
- Malik, A., Witsberger, E., Cottrell, L., Kiefer, A. & Yossuck, P. Perianal Dermatitis, Its Incidence, and Patterns of Topical Therapies in a Level IV Neonatal Intensive Care Unit. Am J Perinatol 35, 486-493, doi:10.1055/s-0037-1608708 (2018).
- Burdall, O., Willgress, L. & Goad, N. Neonatal skin care: Developments in care to maintain neonatal barrier function and prevention of diaper dermatitis. Pediatr Dermatol 36, 31-35, doi:10.1111/pde.13714 (2019).
- Rogers, S., Thomas, M., Chan, B., Hinckley, S. K. & Henderson, C. A Quality Improvement Approach to Perineal Skin Care: Using Standardized Guidelines and Novel Diaper Wipes to Reduce Diaper Dermatitis in NICU Infants. Adv Neonatal Care, doi:10.1097/anc.0000000000000795 (2020).
- Treyvaud, K., Spittle, A., Anderson, P. J. & O'Brien, K. A multilayered approach is needed in the NICU to support parents after the preterm birth of their infant. Early Hum Dev 139, 104838, doi:10.1016/j.earlhumdev.2019.104838 (2019).
- Gerstein, E. D., Njoroge, W. F. M., Paul, R. A., Smyser, C. D. & Rogers, C. E. Maternal Depression and Stress in the Neonatal Intensive Care Unit: Associations With Mother-Child Interactions at Age 5 Years. J Am Acad Child Adolesc Psychiatry 58, 350-358.e352, doi:10.1016/j.jaac.2018.08.016 (2019).
- Lavender, T., Furber, C., Campbell, M., Effect on skin hydration of using baby wipes to clean the napkin area of newborn babies: assessor-blinded randomised controlled equivalence trial. BMC Pediatr 12, 59, doi:10.1186/1471-2431-12-59 (2012).
- Furber, C., Bedwell, C., Campbell, M., The challenges and realties of diaper area cleansing for parents. J Obstet Gynecol Neonatal Nurs 41, E13-25, doi:10.1111/j.1552-6909.2012.01390.x (2012).

Expert care for every delicate skin story
From daily diapering tips to deep dives into skin science, explore our Advice & Care guides and our dedicated Skin Care Hub!💧✨