Select your region
-
Europe
-
Americas
-
Africa and Middle East
-
Asia Pacific
The skin of older adults, characterized by its fragility and increased sensitivity to irritants, requires specialized care to prevent discomfort and skin conditions. Traditional cleaning methods, such as using wipes and tap water, as well as disposable wet wipes containing numerous potentially unnecessary ingredients and additives, raise concerns about hygiene and skin irritation. This study explores the feasibility of using detergent-free or minimally formulated wipes, originally designed for newborn skin, in geriatric settings. Formulated solely with ultrapure water and fruit extract, these wipes exhibit low surface tension, essential for effective cleaning, comparable to that of wipes containing additives. A survey was conducted with 71 residents (n = 71) in four Irish nursing homes, using qualitative methods to assess the experiences of both staff and residents. The results demonstrated that these minimally conditioned wipes were perceived as gentle, effective, and well-suited for incontinence episodes and bed baths. Feedback suggested potential time and cost savings. The wipes were well-received, highlighting their potential as a valuable tool for geriatric care. While further research is needed to validate and expand the application of this method, this study marks a promising development toward innovative approaches to improving the hygiene, comfort, and overall well-being of elderly residents in care facilities through the use of minimally conditioned skin cleansing wipes.
Introduction
The skin of older adults is characterized by its fragility and hypersensitivity, making it particularly vulnerable to aggressions and skin lesions. With age, the skin undergoes significant changes: it thins, loses its elasticity, and thus becomes drier and more delicate (Farage, Miller et al., 2008; Hurlow and Bliss, 2011). This age-related loss of elasticity considerably reduces the skin's viability, often leading to discomfort and skin conditions such as irritation, dermatitis associated with incontinence, and an increased risk of pressure ulcers, particularly among frail residents of nursing homes (Runeman, 2008; Hurlow and Bliss, 2011). Skin cleansing in these populations is generally performed using wipes, tap water and soap, and/or single-use wipes (Al-Samarrai, Uman et al. 2007; Beeckman, Verhaeghe et al. 2011; Groven, Zwakhalen et al. 2017; Veje, Chen et al. 2019; Tai, Hsieh et al. 2021). However, the use of these wipes, which can be used, washed, and reused, carries a risk of infection transmission (Bockmühl, Schages et al. 2019). To circumvent these potential risks, single-use wipes have demonstrated their effectiveness in skin cleansing and are widely used not only in geriatric care (Groven, Zwakhalen et al. 2017, Veje, Chen et al. 2019, Archer, Smyth et al. 2021, Konya, Nishiya et al. 2023) but also in other vulnerable populations such as children and newborns (Price, Lythgoe et al. 2021, Rogers, Thomas et al. 2021).
To effectively cleanse the skin, the liquid component of wipes must have low surface tension (Corazza, Lauriola et al. 2010, Liu 2020). The lower the surface tension, the more easily the liquid spreads on the skin and penetrates deeper into pores and skin folds to trap impurities and debris, thus facilitating their removal (Liu 2020). To reduce surface tension, most commercially available wipes contain surfactants and various other additives (Liu 2020). These effectively lower the surface tension to less than 40 mN/m, allowing for more efficient removal of impurities and debris than cooled boiled water, which typically has a surface tension greater than 70 mN/m. However, these compounds can cause dryness, itching, irritation, and inflammation, which can be exacerbated if residues containing these compounds remain on the skin after use (Aschenbeck and Warshaw 2017, Liu 2020). On mature skin, these adverse effects can have serious consequences if the skin cracks and becomes infected (Surber, Brandt et al. 2015).
A commercially available, detergent-free or minimally formulated wipe containing no surfactants, originally designed for cleansing the delicate skin of newborns, could be suitable for adult use. This wipe contains only ultra-purified water and a fruit extract (with a near-neutral pH), non-irritating ingredients that provide a surface tension equivalent to that of most other wipes on the market, without the addition of surfactants or other additives.
In a prospective study of newborns, minimally formulated wipes demonstrated superiority over two other brands containing significantly more ingredients. The results showed that babies cleaned with minimally formulated wipes were less likely to develop clinically significant irritant diaper rash than those cleaned with the other two brands (Price, Lythgoe et al., 2021). A further evidence-based literature review led to the development of standardized perineal care guidelines that incorporate the use of these minimally formulated wipes. Following the implementation of these guidelines, the incidence of diaper rash decreased by 16.7%, and the incidence of severe cases decreased by 34.9% (n = 1070) (Rogers, Thomas et al., 2021).
After demonstrating their effectiveness in cleansing the skin of newborns, the feasibility of using these minimally conditioned wipes in geriatric settings was assessed. A pilot study was conducted in 2019 in four Irish care facilities to determine whether these detergent-free, minimally conditioned wipes would be more hygienic, more effective, and easier to use than wipes soaked in cooled, boiled water, and gentler on delicate skin than wipes containing surfactants and additives. Here, we present the evidence demonstrating the effectiveness of skin cleansing with a minimally conditioned wipe composed solely of ultrapure water and fruit extract, its application to sensitive skin, and the results of the pilot study.
Reasoning
Low surface tension in liquids is essential for effective skin cleansing, and this is traditionally achieved through the use of surfactants and other additives (Liu 2020). However, even though these wipes containing surfactants may be more effective than cloth and boiled water, there remains a risk of adverse skin reactions and irritation due to the added additives (Liu 2020).
The detergent-free or minimally formulated wipe exhibits a low surface tension comparable to that of wipes containing surfactants and lower than that of boiled tap water, as demonstrated by laboratory tests (Figure 1). This result is achieved through two processes: the use of ultra-purified water and the addition of fruit extract. The proprietary seven-step ultra-purification process of raw water (combining decontamination, filtration, and softening, with the addition of fruit extract) yields a final liquid with a low surface tension (< 35 mN/m), comparable to that of wipes containing additives or surfactants, and significantly lower than that of boiled tap water (> 70 mN/m) (Figure 1.b). (Unpublished data)
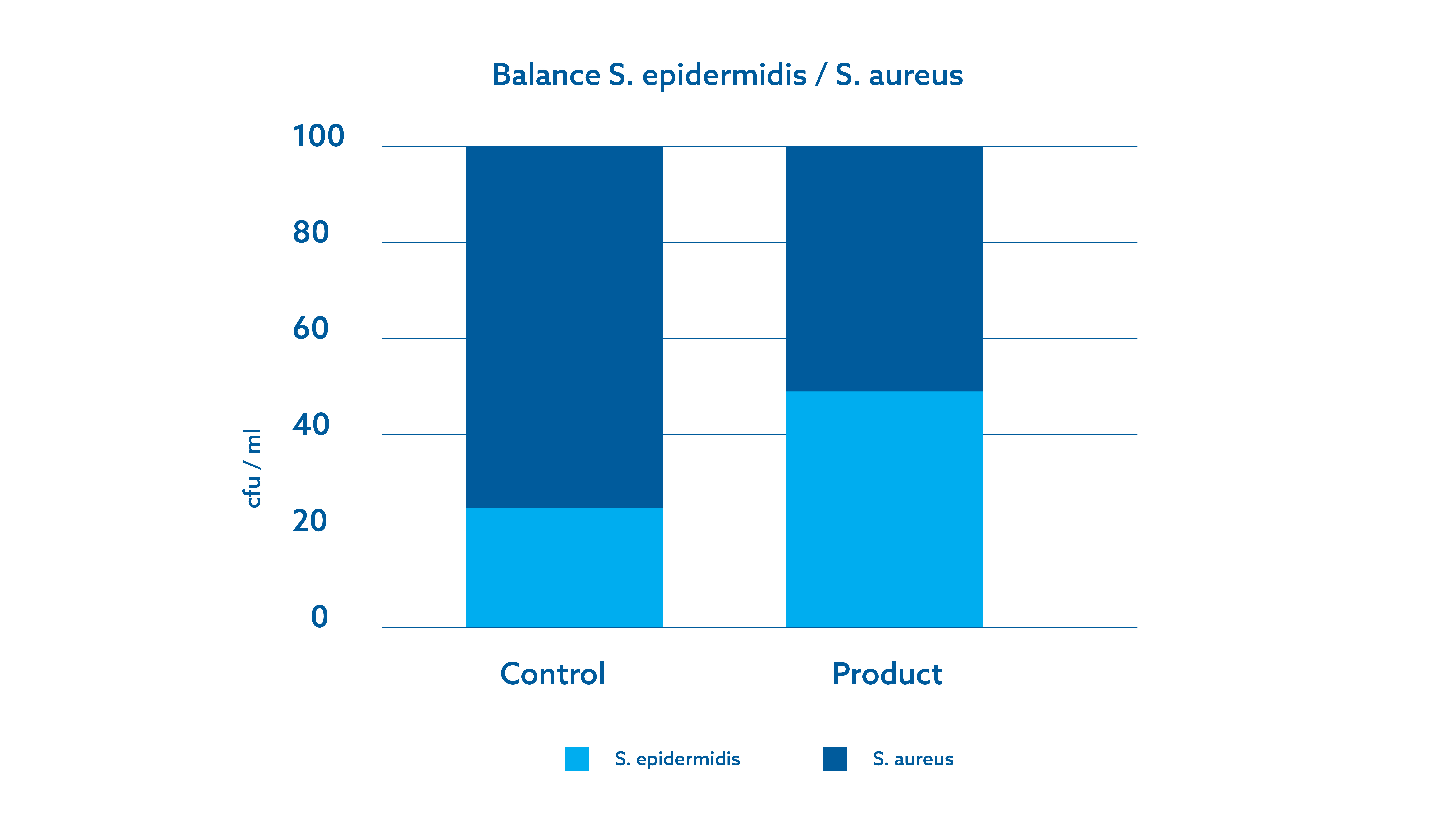
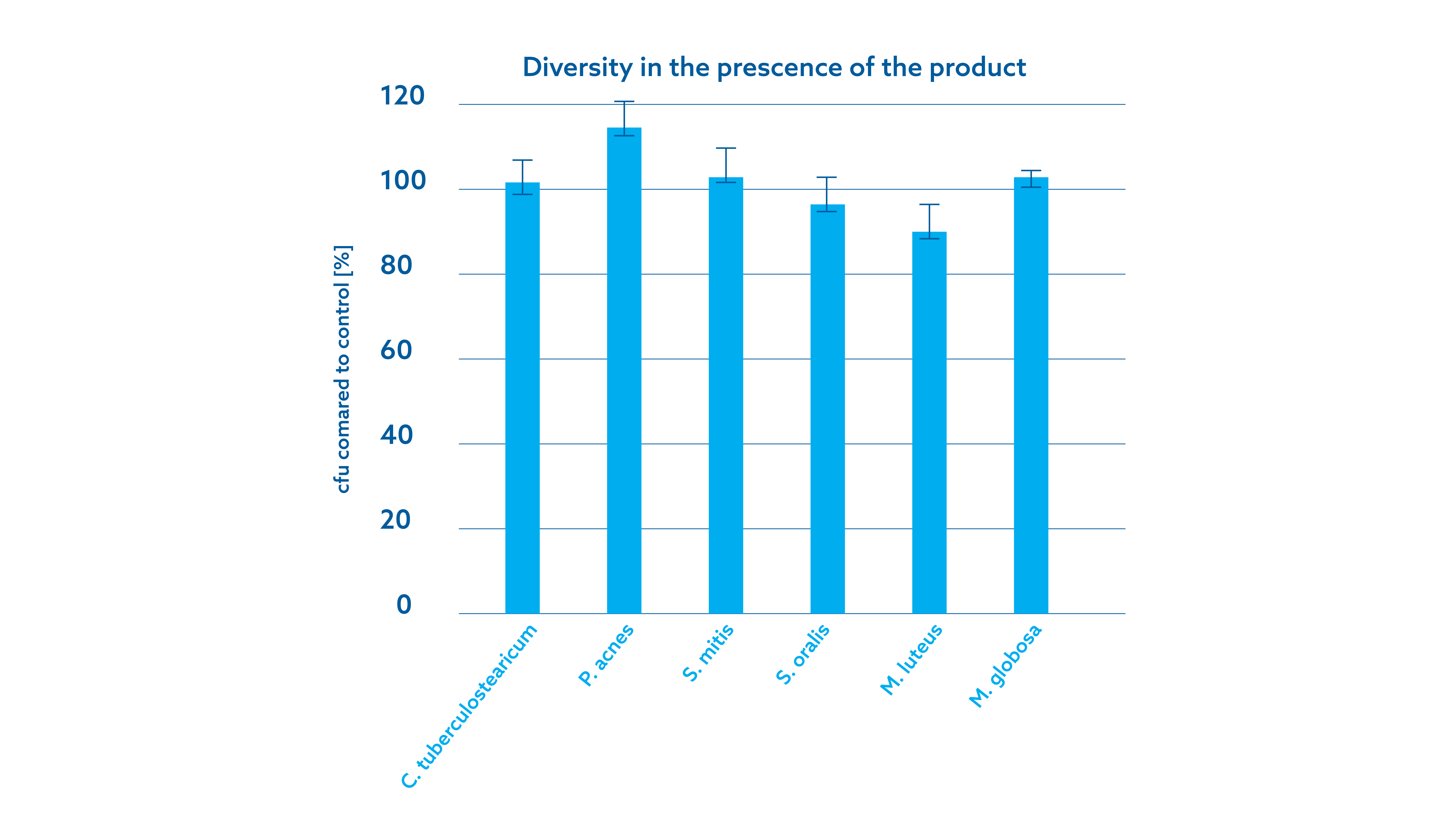
It has also been shown that wipes with minimal ingredients preserve the integrity of the commensal skin flora. Healthy skin is colonized by a diverse community of microorganisms, including bacteria, fungi, and viruses, which collectively constitute the skin flora. These microorganisms create a dynamic ecosystem that forms a protective barrier against pathogens, helps regulate immune responses, and promotes skin homeostasis. The microbiota competes with pathogenic microorganisms for space and nutrients, thus preventing their colonization and the resulting infections (Grice and Segre, 2011). The bacterium Staphylococcus epidermidis produces antimicrobial peptides (bacteriocins) (Newstead, Varjonen et al., 2020) and contributes to maintaining the skin's protective barrier (Zheng, Hunt et al., 2022), thus limiting the proliferation of pathogenic bacteria such as Staphylococcus aureus (Severn and Horswill, 2023). Furthermore, maintaining the diversity of the commensal skin flora helps ensure an optimal pool of protective species (Wallen-Russell 2019). Preserving the natural skin flora and avoiding the routine use of additives that can eliminate the commensal microbiota can help prevent infections (Harris-Ray 2022). A series of certification experiments (Figure 2) demonstrated that minimally invasive wipes do not affect the balance of *S. epidermidis* and *S. aureus* on the skin, nor the diversity of the microbiota. (Unpublished data)
The pilot survey on retirement homes
Background
In geriatric care, ensuring adequate hygiene for residents is essential. Traditionally, care facilities use wipes, dry wipes, and tap water for hygiene. Understanding these practices helped contextualize this pilot study in a nursing home, which aimed to determine whether the current use of minimally invasive wipes for newborns could be adapted for cleaning the skin of elderly individuals.
Methodology
An exploratory qualitative study evaluating the use of detergent-free or minimally formulated wipes for geriatric care was conducted in four nursing homes in Ireland (N = 71 residents, some homes having previously used these wipes, others not). The study had two main objectives: 1) to investigate personal hygiene habits and behaviors prior to the introduction of minimally formulated wipes; and 2) to explore the nursing home staff's experience with these wipes. The study comprised three phases: before, during, and after the trial. It was carried out in four different nursing homes with varying capacities (90, 57, 120, and 29 beds). It is important to note that the study employed a variety of communication methods, both verbal and non-verbal, to accommodate the communication abilities of the participating residents.
During the preliminary phase, an investigator conducted interviews with key staff members at each nursing home. One staff member per nursing home (representing all stakeholders) responded to the investigator, either by completing a questionnaire or by telephone. This initial phase aimed to gather comprehensive information on existing hygiene practices and underlying attitudes regarding the use of cloth wipes, dry wipes and warm water with soap or shower gel, or disposable wet wipes. Attitudes and prior knowledge regarding the use of minimal composition wipes were also collected. During the trial phase, each nursing home received 150 packs of these minimal composition wipes for a three-week period, from January 7 to 29, 2019. During the follow-up phase, feedback was collected approximately ten days after the preliminary interviews, using the same method (one staff member per nursing home representing all stakeholders). This follow-up phase aimed to gather information on the perceived advantages and disadvantages, as well as the different contexts in which the wipes were used. The detergent-free wipes were to be used on all residents of the care facility.
Results and conclusions of the PNHS study
Initially, a study was conducted to understand the residents' current personal hygiene practices. The four nursing homes generally favored the use of cloth wipes or disposable dry wipes, moistened with warm water and shower gel or soap to neutralize odors. Dry wipes were discarded after use, while cloth wipes were washed and reused.
The study gathered positive feedback regarding the use of detergent-free or minimally formulated wipes in geriatric care. These wipes were rated as soft, non-abrasive, and high-quality, fragrance-free, and non-drying. They also proved effective for cleansing skin during incontinence episodes and bed baths, requiring less equipment than traditional methods such as dry wipes and hot water, as they are more effective from the first wash. The practicality, quality, and effectiveness of the wipes were identified as key factors for decision-makers in nursing homes. Some participants expressed mixed opinions regarding the wipes' moisture content, noting that additional drying was necessary after use. Prior to the trial, staff were instructed to pat the skin dry (rather than wiping it) with a clean, dry towel or a dry wipe if needed, to avoid irritation. Furthermore, some participants reported a feeling of coldness when using these minimal composition wipes.
The study demonstrated that detergent-free or minimally formulated wipes offered a potential solution for reducing the time spent on hygiene care, particularly in cases of incontinence and for bed baths. Their use was also suggested in other areas of nursing homes, such as the dining room for cleaning faces and hands before and after meals, and the art studio for removing hand paint. Importantly, no nursing home reported any adverse skin reactions following the use of these wipes.
The PNHS study demonstrated that minimally invasive wipes can be a valuable asset for geriatric care in nursing homes. Their practicality, quality, and effectiveness make them an attractive option for improving hygiene and the overall well-being of elderly residents. Positive feedback and the willingness of nursing homes to continue using these wipes after the trial suggest a promising future for their adoption in geriatric care.
Discussion
Positive feedback from caregivers and residents regarding these minimally nutrient wipes highlights their potential as a valuable tool for cleansing the skin of elderly individuals. These wipes have proven effective in thoroughly cleaning pores and skin folds, particularly during episodes of incontinence and bed baths, thus reducing the time spent on these essential hygiene practices. This aligns with the broader objective of improving the quality of care provided to elderly residents in nursing homes. Furthermore, their superior effectiveness during the initial cleansing (compared to dry wipes and hot water) could lead to a reduction in the quantity of wipes used and the cleaning time required, resulting in cost savings and reduced waste for care facilities.
These results indicate that the use of minimally invasive wipes in geriatrics confirms the findings of previous research highlighting their potential benefits in neonatology. Data from previous studies on the preservation of natural skin flora by these wipes could indirectly contribute to preventing opportunistic skin infections in older adults. Their ability to achieve low surface tension without the use of surfactants perfectly aligns with the objective of minimizing potential irritants that could negatively affect skin aging.
This exploratory PNHS study had some limitations. Conducted in a small sample of Irish long-term care facilities, it requires a broader scope to determine whether its results are representative of other care settings. Furthermore, while the study elicited positive feedback and an intention to continue using the wipes, longer-term post-trial observations would provide a better understanding of the wipes' lasting impact on skin health, resident comfort, ease of use for caregivers, and cost-effectiveness.
Future research, conducted using a more rigorous methodology, could broaden the scope of the study to include a larger number of care and residential facilities for the elderly, with a particular focus on episodes of incontinence and associated dermatitis. Longitudinal studies evaluating the effects of minimally conditioned wipes on skin health and overall well-being could provide valuable information on their potential long-term benefits. Direct comparative studies, contrasting these wipes with traditional wipes containing surfactants and with cloth methods, would help to better define their advantages and limitations.
Conclusion
In conclusion, the positive results of this PNHS study offer a promising glimpse into the potential of detergent-free or minimally nutrient-dense wipes in geriatric care. These wipes could improve hygiene, reduce discomfort, and optimize the overall quality of care provided to older adults. The study's findings align with the growing recognition of the importance of preserving the skin microbiome and minimizing potential irritants, particularly for fragile and sensitive skin associated with aging. While further research is needed to validate and expand upon these results, this study paves the way for the adoption of innovative approaches in geriatric skincare, thereby contributing to the well-being and comfort of older adults in care facilities.
References
- Al-Samarrai, NR, GC Uman, T. Al-Samarrai and CA Alessi (2007). "Introduction of a new incontinence management system for nursing home residents." J Am Med Dir Assoc 8 (4): 253-261.
- Archer, V., W. Smyth and C. Nagle (2021). "Bath wipes, a valuable hygiene option for frail older adults at home: a proof-of-concept study." Australian Journal of Advanced Nursing 38 (3).
- Aschenbeck, KA and EM Warshaw (2017). “Allergenic ingredients in personal hygiene wet wipes.” Dermatitis 28 (5): 317-322.
- Beeckman, D., S. Verhaeghe, T. Defloor, L. Schoonhoven and K. Vanderwee (2011). "A 3-in-1 perineal washcloth impregnated with 3% dimethicone versus water and pH-neutral soap for preventing and treating incontinence-associated dermatitis: a randomized controlled clinical trial." J Wound Ostomy Continence Nurs 38 (6): 627-634.
- Bockmühl, DP, J. Schages and L. Rehberg (2019). “Linen and textile hygiene in the health sector and beyond.” Microb Cell 6 (7): 299-306.
- Corazza, M., MM Lauriola, M. Zappaterra, A. Bianchi and A. Virgili (2010). “Surfactants, protagonists of skin cleansing.” J Eur Acad Dermatol Venereol 24 (1): 1-6.
- Farage, MA, KW Miller, P. Elsner and HI Maibach (2008). "Intrinsic and extrinsic factors of skin aging: a review." Int J Cosmet Sci 30 (2): 87-95.
- Grice, EA and JA Segre (2011). "The skin microbiome." Nat Rev Microbiol 9 (4): 244-253.
- Groven, FM, SM Zwakhalen, G. Odekerken-Schröder, EJ Joosten and JP Hamers (2017). "How does waterless washing compare with traditional bed bathing: a systematic review." BMC Geriatr 17 (1): 31.
- Harris-Ray, N. (2022). "What is the difference between antibacterial soap and plain soap?" Retrieved August 18, 2023 from https://www.webmd.com/a-to-z-guides/difference-between-antibacterial-soap-plain-soap .
- Hurlow, J. and DZ Bliss (2011). “Dry skin in the elderly.” Geriatr Nurs 32 (4): 257-262.
- Konya, I., K. Nishiya, I. Shishido, M. Hino, K. Watanabe and R. Yano (2023). "Minimum wiping pressure and number of wipes required to remove soiling during bed baths using disposable towels: a multi-study approach." BMC Nurs 22 (1): 18.
- Liu, L. (2020). “Skin penetration of surfactants.” J Cosmet Sci 71 (2): 91-109.
- Newstead, LL, K. Varjonen, T. Nuttall and GK Paterson (2020). “Bacteriocins and antimicrobial peptides produced by staphylococci: their potential as alternative treatments for Staphylococcus aureus infections.” Antibiotics (Basel) 9 (2).
- Price, AD, J. Lythgoe, J. Ackers-Johnson, PA Cook, AM Clarke-Cornwell, and F. MacVane Phipps (2021). "BaSICS (Baby Skin Integrity Comparison Survey): A prospective experimental study using maternal observations to report the effect of baby wipes on the incidence of irritant diaper dermatitis in infants from birth to eight weeks." Pediatr Neonatol 62 (2): 138-145.
- Rogers, S., M. Thomas, B. Chan, SK Hinckley, and C. Henderson (2021). "A quality improvement approach to perineal skin care: Use of standardized guidelines and novel diaper wipes to reduce diaper dermatitis in neonatal intensive care infants." Adv Neonatal Care 21 (3): 189-197.
- Runeman, B. (2008). "Skin interaction with absorbent hygiene products." Clin Dermatol 26 (1): 45-51.
- Severn, MM and AR Horswill (2023). "Staphylococcus epidermidis and its dual lifestyle in skin health and infection." Nat Rev Microbiol 21 (2): 97-111.
- Surber, C., S. Brandt, A. Cozzio and J. Kottner (2015). “Principles of skin care in the elderly.” G Ital Dermatol Venereol 150 (6): 699-716.
- Tai, CH, TC Hsieh and RP Lee (2021). "The effect of bed bathing practices on costs and vital signs of critically ill patients." Int J Environ Res Public Health 18 (2).
- Veje, PL, M. Chen, CS Jensen, J. Sørensen and J. Primdahl (2019). "Bed bathing with soap and water or disposable wet wipes: patient experiences and preferences." J Clin Nurs 28 (11-12): 2235-2244.
- Wallen-Russell, C. (2019). "The role of daily cosmetics in modifying the skin microbiome: a study using biodiversity." Cosmetics 6 (1): 2.
- Archived WaterWipes data.
- Zheng, Y., RL Hunt, AE Villaruz, EL Fisher, R. Liu, Q. Liu, GYC Cheung, M. Li and M. Otto (2022). "Commensal Staphylococcus epidermidis contributes to skin barrier homeostasis by generating protective ceramides." Cell Host Microbe 30 (3): 301-313.e309.
legends of the figures
Figure 1. Internal data: (A) Illustrates the influence of surface tension on a liquid's ability to spread on the skin and penetrate crevices and pores; (B) Surface tension differences between the minimal ingredients wipe at room temperature, tap water at room temperature, and boiled tap water at room temperature; (C) Surface tension differences between the minimal ingredients wipe and other skin cleansers. TA = room temperature.

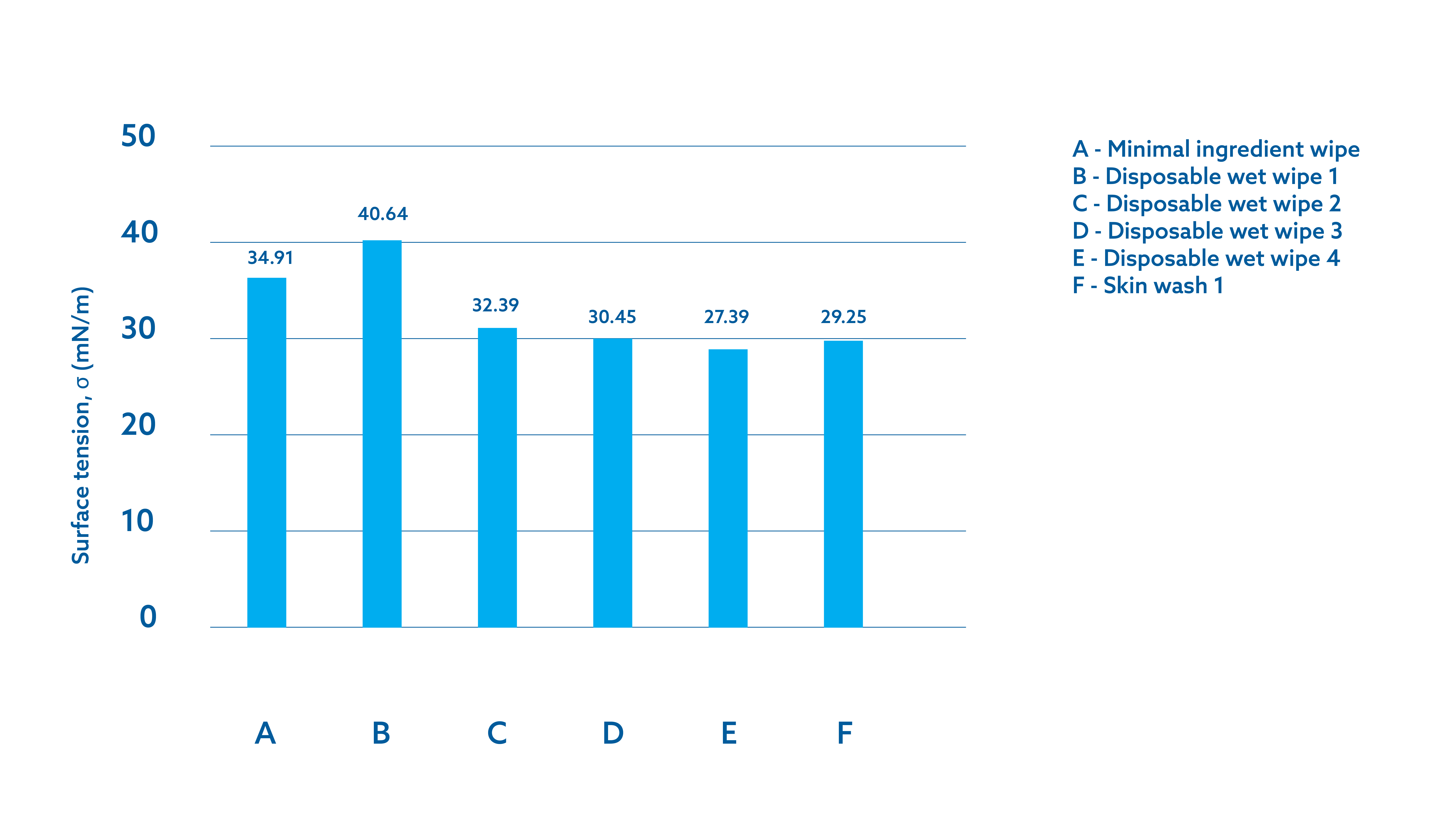

Figure 2. Archived data (A) The balance between Staphylococcus epidermidis and Staphylococcus aureus during incubation with a phosphate-buffered saline control compared to the minimal ingredients wipe; (B) The diversity of organisms composing the skin microbiome in the presence of the minimal ingredients wipe (dry skin).

Expert care for every delicate skin story
From daily diapering tips to deep dives into skin science, explore our Advice & Care guides and our dedicated Skin Care Hub!💧✨


